MCB TRANSCRIPT

Tuberculosis: Dislodging a Tenacious Pathogen
Tuberculosis is hard to shake. The bacterium that causes it — Mycobacterium tuberculosis — infects a third of people worldwide, can live in us for decades with no symptoms, and has been with us for nearly 40,000 years. "It has evolved not to kill us," says MCB Professor Jeffery Cox. "It tempers its virulence, entering our bodies and thwarting our immune systems."

TB's ability to lay low also helps it resist antibiotics, making it extremely difficult to treat. To find better treatments, Cox studies how TB evades the immune response in mice as well as in mouse and human cells. While at UCSF, he began working with MCB researchers Dan Portnoy, Russell Vance, Greg Barton, and Sarah Stanley, and is happy to be joining them on campus. "They're some of my best and closest collaborators," he says. "We all study different bacteria that infect macrophages and share our data. This synergy leads to incredible headway."
Macrophages, a kind of white blood cell that ingests pathogens, seal TB in vesicles made from the cell membrane called phagosomes. "My MCB collaborators helped me discover that when TB is pathogenic, it punches holes in the phagosome membrane," Cox says. This provides access to host cell nutrients and lets the bacterium manipulate its host.
He then found that the holes are poked by ESX-1 — an export system that secretes TB proteins into host cells — and that those holes somehow alert the cell to the fact that it's infected with a pathogen. "Lots of bacteria poke holes in this membrane, and the macrophage detects this pattern," he explains. "It doesn't need to identify the pathogen to respond."
Now Cox is investigating how TB and the host respond to each other during infection. So far, he's found three main pathways. When TB punches holes in a phagosome, macrophages target it for destruction by an enzyme-filled organelle called a lysosome. Cox likens the fact that macrophages respond to active but not inactive TB to DEFCON, the U.S. Defense Condition system of matching military readiness to threat levels.
Macrophages can also commit suicide, thereby killing the TB inside them. And Cox has found a way the TB can outwit the host. M. tuberculosis DNA mimics that of a virus, tricking the host into activating its antiviral response. But the inappropriate antiviral response actually inhibits an effective immune response against TB. However, when mice lack the antiviral immune gene, their immune response to TB does increase.
Cox will also direct UC Berkeley's Center for Emerging & Neglected Diseases. "TB is a neglected disease," he points out. "It's not profitable to make drugs for it because it afflicts mostly poor, developing countries." Besides being a good fit with his research, this is an issue his childhood in Kenya made him care about.
And as if he needed yet another reason to join MCB, he was an undergraduate at UC Berkeley in Marian Koshland’s lab. Says Cox, "I’m excited to be coming home."
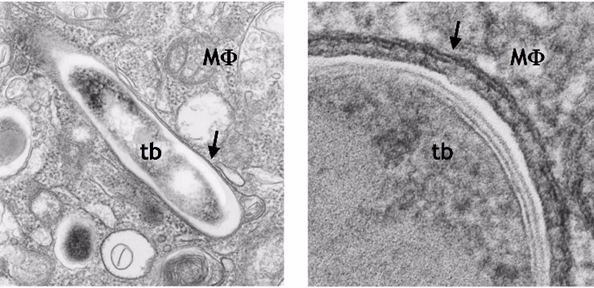
when tuberculosis is active, it pokes holes in the phagosome membrane (arrows).




