MCB TRANSCRIPT

Neural Networks: Restoring Balance in Epilepsy and Autism
A delicate balance of excitation and inhibition normally keeps neural networks humming along, but throwing them off balance can cause neural diseases. To find out how, MCB Assistant Professor Helen Bateup studies a protein complex — the tuberous sclerosis complex (TSC) — that controls excitability in neurons and that is linked to neural disorders. Most people with TSC mutations have epilepsy and about half also have autism.

Epilepsy is caused by hyperexcitability of neural circuits, often in a brain region called the hippocampus. As a post-doc, Bateup discovered that TSC mutations decrease inhibition in the hippocampus, increasing excitability of the hippocampal network and causing seizures. She also found that this is due to increased activity of another protein complex, called mammalian target of rapamycin (mTOR). But we don’t know which part of the TSC/mTOR pathway affects neural networks in the hippocampus.
“It’s a big black box,” Bateup says. “Something downstream of mTOR is regulating inhibition.”
To find out what, she’s testing whether TSC mutations decrease the number or function of inhibitory receptors on hippocampal neurons in mice, as well as screening broadly for molecular alterations in these cells. Her work could lead to more targeted treatments for epilepsy. While mTOR inhibitors may help treat this disorder, they also have debilitating side effects because mTOR regulates many cellular processes in and outside of the brain.
As a graduate student, Bateup studied another brain region called the basal ganglion that is implicated in autism. Now, she’s investigating whether the TSC/mTOR pathway also affects neurons in this part of the brain, using mice with TSC mutations in specific kinds of basal ganglia neurons. “If we can identify the cell types and circuits perturbed by these mutations, we may be able to treat those instead of the entire brain,” she says.
But mouse studies will only get you so far. “Are there the same changes in human neurons as in mouse neurons?” Bateup asks. One way to find out is in cells from patients with TSC mutations. “The trick is you can take skin cells, which is not invasive, and transform them into neurons,” she explains. This technique also lets her introduce normal TSC genes into patient cells to see if that can restore proper function.
“Our goal is to understand the connection between the TSC/mTOR pathway and neural diseases at the molecular, cellular and behavioral levels,” Bateup says. “If we can link these, it will be very satisfying.”
Bateup has recently received the 2014 Regents' Junior Faculty Fellowship and a 2015 Sloan Research Fellowship.
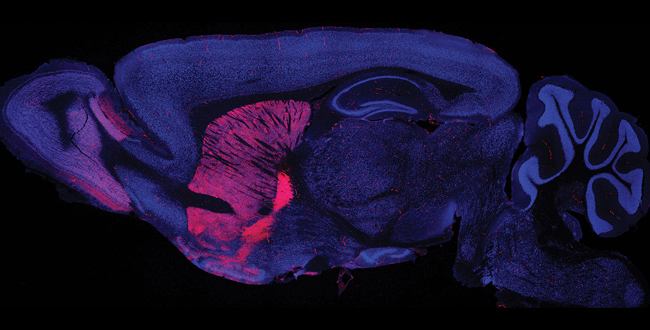
with a selectively mutated TSC gene in the basal ganglia.




